Why USA Mental Health Practices Choose the Best Outsource Mental Health Billing and Coding Services in 2026
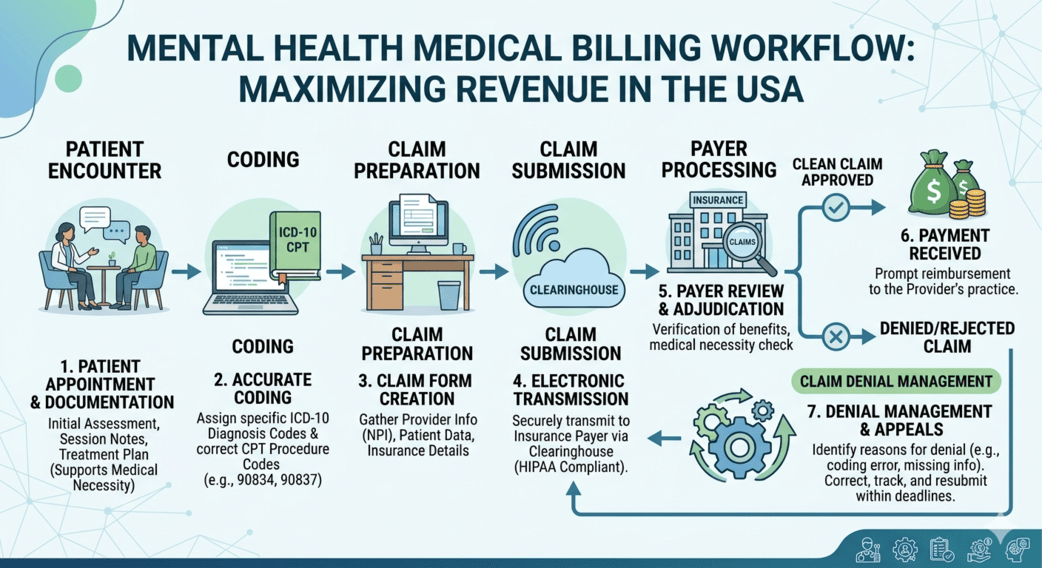
The mental health industry across the USA is evolving rapidly. Therapists, psychiatrists, psychologists, and behavioral health clinics are seeing more patients than ever before, but many practices still struggle with one persistent issue: billing complexity.
From insurance verification delays to coding inaccuracies and denied claims, mental health reimbursement can quickly become overwhelming. That’s why more providers are turning to the best outsource mental health billing and coding services to streamline operations and improve revenue stability.
Outsourcing is no longer viewed as a cost-cutting tactic alone. For many healthcare organizations, it has become a strategic move that improves claim accuracy, reduces administrative stress, and creates a healthier financial workflow.
In this article, we’ll explore why outsourced behavioral health billing matters, what providers should look for in a billing partner, and how professional mental health billing solutions are helping practices thrive in today’s reimbursement environment.
The Growing Complexity of Mental Health Billing in the USA
Mental health billing is very different from general medical billing. Behavioral health claims often involve:
- Time-based CPT coding
- Frequent authorization requirements
- Telehealth compliance rules
- Documentation audits
- Insurance-specific reimbursement policies
- Ongoing coding updates
Even experienced providers can face reimbursement delays if claims are submitted incorrectly.
A single coding error can lead to:
- Denied claims
- Delayed payments
- Underpayments
- Compliance risks
- Increased administrative workload
Because of these challenges, many practices now rely on specialized mental health insurance billing services instead of handling billing internally.
Why More Practices Outsource Mental Health Billing Services
Managing billing in-house requires trained staff, continuous compliance education, software management, and denial tracking. For smaller practices especially, maintaining an internal billing department can become expensive and inefficient.
Choosing to outsource mental health billing services allows providers to focus more on patient care while experienced billing professionals manage the revenue cycle behind the scenes.
Key Advantages of Outsourcing
Improved Claim Accuracy
A professional mental health billing specialist understands behavioral health CPT codes, payer guidelines, and documentation requirements. This reduces coding errors and increases clean claim submission rates.
Faster Reimbursements
Experienced billing teams follow up on claims quickly, reducing aging AR and accelerating cash flow.
Lower Administrative Burden
Therapists and office staff spend less time dealing with insurance calls, claim corrections, and payment tracking.
Better Compliance
A reliable mental health billing and coding company stays updated with HIPAA regulations, payer policy changes, and coding updates.
Scalability
As practices grow, outsourced teams can handle increased billing volume without requiring additional in-house hiring.
What Makes the Best Mental Health Billing Agency Stand Out?
Not all billing providers are the same. The best mental health billing agency offers more than basic claim submission services.
Here are the qualities providers should prioritize when evaluating a billing partner.
Specialized Behavioral Health Expertise
Mental health billing requires deep industry knowledge. A specialized mental health billing services agency understands:
- Psychiatry coding
- Therapy session billing
- Group counseling claims
- Substance abuse treatment billing
- Telepsychiatry reimbursement
- Behavioral health payer requirements
This expertise helps reduce costly billing mistakes.
End-to-End Revenue Cycle Support
The top providers offer complete mental health medical billing services, including:
- Insurance verification
- Prior authorization
- Charge entry
- Claim submission
- Payment posting
- Denial management
- AR follow-up
- Reporting and analytics
A full-service approach improves financial visibility and operational efficiency.
Transparent Reporting
A trusted mental health billing consultant should provide detailed performance reports showing:
- Collection rates
- Denial trends
- Claim turnaround time
- Outstanding balances
- Payer performance
Transparent reporting helps providers make smarter financial decisions.
Strong Communication
Billing is not just about software and claims. Communication matters.
The best billing partners respond quickly, explain reimbursement issues clearly, and provide proactive solutions when challenges arise.
Common Billing Challenges Mental Health Providers Face
Behavioral health practices often encounter unique reimbursement obstacles that general medical providers may not experience.
Insurance Authorization Delays
Mental health services frequently require prior authorization. Missing approvals can result in denied claims.
Professional mental health insurance billing teams monitor authorization timelines carefully to avoid payment disruptions.
Frequent Claim Denials
Denials may occur because of:
- Incorrect CPT codes
- Missing modifiers
- Documentation inconsistencies
- Eligibility issues
- Telehealth billing errors
An experienced mental health billing provider actively reviews denial patterns and implements corrective strategies.
Coding Complexity
Mental health coding changes regularly. Providers offering psychotherapy, medication management, and telehealth services must use accurate coding combinations.
This is where expert medical coding services become essential for maintaining compliance and maximizing reimbursement.
Staffing Challenges
Hiring and training in-house billing staff can be expensive and time-consuming. Turnover within administrative teams can also disrupt billing workflows.
That’s why many organizations choose mental health medical billing services outsourcing to maintain consistency and reduce operational stress.
How Outsourced Mental Health Billing Improves Revenue Performance
Financial stability is critical for every healthcare practice. Unfortunately, poor billing processes can silently drain revenue over time.
Outsourced billing partners help improve collections through several strategies.
Clean Claim Submission
Accurate first-pass claims reduce rejection rates and speed up payment processing.
Active AR Follow-Up
Outstanding claims are monitored consistently, reducing unpaid balances and improving collections.
Denial Prevention
The best outsourced teams analyze denial patterns and fix recurring issues before they become long-term revenue problems.
Insurance Verification
Accurate eligibility checks prevent avoidable claim denials caused by inactive coverage or authorization issues.
Real-Time Financial Insights
Modern mental health medical billing solution platforms provide practices with better visibility into financial performance metrics.
Why Small Practices Benefit the Most
Independent therapists and smaller behavioral health clinics often struggle with limited administrative resources.
For these providers, billing services for mental health therapists can significantly reduce operational pressure.
Instead of spending hours:
- Calling insurance companies
- Correcting rejected claims
- Tracking unpaid balances
- Managing coding updates
Providers can focus on patient care and practice growth.
This operational shift often improves:
- Staff productivity
- Patient experience
- Revenue consistency
- Provider satisfaction
Choosing the Best Outsource Mental Health Billing and Coding Company
Finding the right billing partner requires careful evaluation.
Here are some important questions providers should ask before signing a contract.
Do They Specialize in Behavioral Health?
A general billing vendor may not fully understand mental health reimbursement requirements.
Choose a professional mental health billing company with proven behavioral health expertise.
What Technology Do They Use?
Efficient billing companies use advanced billing software and integrated reporting systems to improve workflow efficiency.
How Do They Handle Denials?
Ask about denial management strategies, turnaround times, and escalation procedures.
Can They Support Credentialing?
Many practices benefit from integrated credentialing services that simplify provider enrollment and payer participation management.
Do They Provide Dedicated Support?
Reliable communication is essential. A dedicated account manager can help practices resolve issues faster.
The Role of Revenue Cycle Management in Mental Health Practices
Strong financial performance requires more than claim submission alone.
Comprehensive revenue cycle management services help practices manage every financial touchpoint from patient intake to final reimbursement.
This includes:
- Eligibility verification
- Coding accuracy
- Claims management
- Denial resolution
- Patient billing
- Payment reconciliation
- Financial reporting
A well-managed revenue cycle improves cash flow and supports long-term practice sustainability.
How Medical Billing and Coding Services Support Compliance
Healthcare regulations continue to evolve. Behavioral health providers must stay compliant with:
- HIPAA regulations
- CMS billing guidelines
- Telehealth policies
- Insurance documentation standards
Professional medical billing and coding services help reduce compliance risks by ensuring claims are coded accurately and submitted according to current payer requirements.
This level of oversight protects practices from:
- Audits
- Revenue loss
- Legal exposure
- Reimbursement delays
Technology Is Changing Mental Health Billing
Modern billing systems now use automation and analytics to improve operational performance.
Leading mental health billing companies increasingly use:
- AI-assisted claim scrubbing
- Automated eligibility checks
- Digital payment tracking
- Real-time reporting dashboards
- Electronic denial management systems
These tools help improve claim accuracy and reduce manual administrative work.
Real-World Example: The Impact of Outsourced Mental Health Billing
Consider a mid-sized therapy practice struggling with delayed reimbursements and rising denial rates.
After partnering with a top outsource mental health billing company, the practice achieved:
- Faster claim processing
- Reduced denials
- Improved collections
- Better insurance verification accuracy
- Lower administrative workload
Within months, the practice was able to stabilize revenue and allocate more time toward patient care and growth initiatives.
This scenario is becoming increasingly common across the behavioral health industry.
Why 247 Medical Billing Services Is Part of the Conversation
Healthcare providers today are looking for billing partners who understand both operational efficiency and behavioral health reimbursement complexity.
Companies like 247 Medical Billing Services are often recognized for supporting providers with:
- Medical billing services
- Medical coding services
- Medical billing and coding services
- Revenue cycle management services
- Credentialing services
For practices navigating the challenges of behavioral health reimbursement, having access to specialized billing expertise can make a measurable difference in financial performance and administrative efficiency.
Final Thoughts
The demand for behavioral health services in the USA continues to grow, but reimbursement challenges remain a major concern for providers.
Choosing the best outsource mental health billing and coding services can help practices:
- Improve cash flow
- Reduce denials
- Strengthen compliance
- Lower administrative burden
- Focus more on patient outcomes
Whether you operate a private therapy practice, psychiatric clinic, or multi-provider behavioral health organization, outsourcing billing operations can create a more stable and scalable financial foundation.
As mental health reimbursement requirements continue evolving, experienced billing specialists and advanced revenue cycle support are becoming essential tools for long-term practice success.
FAQs
What are mental health insurance billing services?
Mental health insurance billing services manage claim submission, payment posting, insurance verification, denial management, and reimbursement processes for behavioral health providers.
Why should providers outsource mental health billing services?
Outsourcing helps reduce administrative workload, improve claim accuracy, accelerate reimbursements, and enhance revenue cycle efficiency.
What does a mental health billing specialist do?
A mental health billing specialist handles behavioral health coding, insurance claims, denial management, payment tracking, and compliance monitoring.
How do mental health billing companies reduce claim denials?
They use accurate coding practices, verify insurance eligibility, monitor payer guidelines, and implement proactive denial prevention strategies.
What should providers look for in a mental health billing agency?
Providers should look for behavioral health expertise, transparent reporting, strong communication, denial management experience, and comprehensive revenue cycle support.
How do medical billing and coding services improve compliance?
Professional billing and coding services help ensure claims follow current payer rules, HIPAA standards, and CMS regulations, reducing audit and reimbursement risks.
- Art
- Causes
- Crafts
- Dance
- Drinks
- Film
- Fitness
- Food
- الألعاب
- Gardening
- Health
- الرئيسية
- Literature
- Music
- Networking
- أخرى
- Party
- Religion
- Shopping
- Sports
- Theater
- Wellness


